What is chickenpox?
Chickenpox is a highly contagious virus infection that causes a acute fever and blisters eruption, mainly in children.
The name may be derived from the French term for chickpea, chiche pois. Another theory is that the word 'chicken' is derived from a slang term for 'boy'. Chickenpox is also known as chickenpox.
Who is at risk for chickenpox?
Chickenpox occurs worldwide and affects people of all races, sex and age. However, most cases occur in children before the age of ten.
Once a person has had chickenpox infection, they are unlikely to get it again, as it confers lifelong immunity.
Immunocompromised People are susceptible to the virus at all times and must take steps to prevent or modify the course of the disease if there has been exposure to the virus.
What is the cause of chickenpox?
Chickenpox is caused by primary infection with the varicella-zoster virus, Herpesviridae family. This virus is sometimes called herpesvirus type 3.
How is chickenpox contracted?
Chickenpox is highly contagious and is easily transmitted from person to person by breathing respiratory droplets into the air from an infected person's cough or sneeze, or by direct contact with fluid from open sores.
A person who is not immune to the virus has a 70–80% chance of becoming infected with the virus if exposed in the early stages of the disease.
What are the signs and symptoms of chickenpox?
In children, chickenpox usually starts with a red itch. papules progressing to vesicles in the stomach, back and face, and then spreads to other parts of the body. Blisters can also arise inside the mouth.
The spread pattern may vary from child to child. There may be only one dispersion of vesicles, or the entire body may be covered with up to 500 vesicles. The vesicles tend to be very itchy and uncomfortable.
Some children may also experience additional symptoms such as high fever, headache, cold-like symptoms, vomiting, and diarrhea.
Chickenpox is usually more severe in adults and can be fatal in complicated cases. Most adults who have experience with chickenpox prodromal symptoms for up to 48 hours before erupting into the rash. These include fever, discomfort, headache, loss of appetite and abdominal pain. Chickenpox is usually more severe in adults and can be fatal in complicated cases.
The blisters disappear in one to three weeks, but they can leave some scars. Most often they are depressed (anetoderma), but may be thickened (hypertrophic scars) Scarring is prominent when the lesions become infected with bacteria.
Chickenpox
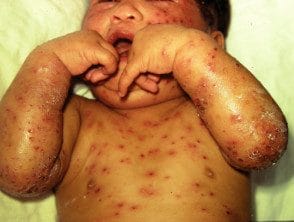
Chickenpox
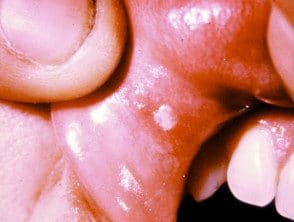
Chickenpox
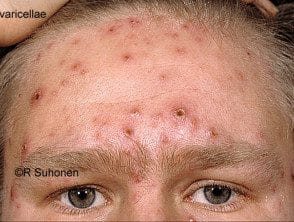
Chickenpox
See more chickenpox images ...
How is chickenpox diagnosed?
Diagnosis of chickenpox is usually made in the presence of its characteristic rash and the presence of different stages of lesions simultaneously. One clue to diagnosis is knowing that the patient has been exposed to an infected contact within 10 to 21 days. incubation period. Patients may also have prodromal signs and symptoms. See also chickenpox. pathology.
Laboratory tests are often done to confirm the diagnosis.
- PCR Detects chickenpox virus in skin lesions and is the most accurate method of diagnosis.
- the culture of fluid from the blister takes a long time and is done less often.
- Serology (IgM and IgG) is more useful in pregnant women or before prescribing immunosuppression medication to determine the need for immunization prior to treatment.
What are the complications of chickenpox?
In healthy children, chickenpox infection is usually a self-limiting, uncomplicated disease. Complications can include:
- Secondary bacterial infection of skin lesions caused by scratching
- Infection can lead to abscesscellulitis necrotizing fasciitis and gangrene
- Dehydration from vomiting and diarrhea.
- Exacerbation asthma
- Viral pneumonia
Some complications are seen more frequently in immunosuppressed patients and adults with chickenpox.
- Disseminated primary chickenpox infection; this carries high morbidity
- Central nervous system complications like Reye syndromeGuillain-Barré syndrome and encephalitis
- Thrombocytopenia and purple
Chickenpox in pregnancy
- Non-immune pregnant women should be careful to avoid contact with people who have chickenpox and wash their hands frequently when handling food, animals, and children. Exposure to the chickenpox virus in pregnancy can cause viral pneumonia, premature labor and delivery, and rarely maternal death.
- Approximately 25% from fetuses of mothers with chickenpox become infected. It is harmless to most of them. The offspring can remain asymptomaticor developing herpes zoster at a young age with no history of primary chickenpox infection. They can also develop congenital Chickenpox syndrome, one of the TORCH infections.
- Congenital chickenpox syndrome occurs in up to 2% of fetuses exposed to chickenpox in the first 20 weeks of gestation. May cause miscarriage, fetal chorioretinitis, waterfallstip atrophy, cerebral cortical atrophy and microcephaly, cutaneous scars and neurological disability.
- Mortality in newborns infected with chickenpox is up to 30%.
Perinatal chicken pox
- If a mother develops chickenpox just before delivery or within 28 days after delivery, her baby is at risk of a serious infection.
Herpes zoster (Herpes zoster)
- Varicella-zoster virus remains dormant in sensory ganglia after infection
- It can reactivate after many years as herpes zoster. Herpes zoster presents grouped vesicular injuries, usually involving only one dermatome.
- Other infections that occur as a result of virus reactivation include post-herpetic. neuralgia, vasculopathyretinal myelopathy necrosis, cerebelitis and sinusoidal herpes zoster.
What is the treatment for chickenpox?
For most healthy chickenpox patients, symptomatic therapy is usually all that is required.
- Trim children's nails to minimize scratching.
- Take a warm bath and apply hydration. cream.
- Acetaminophen can reduce fever and pain (do not use aspirin in children, as this is associated with Reye's syndrome).
- Calamine lotion and oral antihistamines can relieve itching.
- Consider oral acyclovir (antiviral agent) in people older than 12 years, which reduces the number of days with fever.
Immunosuppressed patients with chickenpox need intravenous treatment with the antiviral acyclovir.
In cases of involuntary exposure to the virus, varicella-zoster immunoglobulin, if administered within 96 hours after initial contact, may reduce the severity of the disease, but not prevent it. This is used where there is no history of chickenpox (or the patient has no antibodies to varicella-zoster virus in blood tests) in pregnancy, in the first 28 days after delivery and in immunodeficient or immunosuppressed patients.
How to prevent the spread of chickenpox
A person with chickenpox is contagious 1–2 days before the rash appears and until all blisters have crusted over. This can take 5-10 days. Children should be kept away from school or daycare during this contagious period. Adults with chickenpox who work among children should also stay home.
It may take 10 to 21 days after contact with an infected person for someone to develop chickenpox. This is the time it takes for the virus to replicate and erupt in the characteristic rash on the new host.
Because chickenpox can cause complications in immunocompromised individuals and pregnant women, these people should avoid visiting friends or family when a case of chickenpox is known. In case of involuntary contact, consult your doctor, who can prescribe special preventive treatment.
Chickenpox vaccination
The vaccine is available for chickenpox and is highly recommended.
Chickenpox is highly preventable by vaccination with the live attenuated chickenpox vaccine. The vaccine is subsidized (“scheduled”) for 15-month-old babies in New Zealand, as well as for non-immune individuals who are immunosuppressed or are in other special groups. If you are in New Zealand, consult the Immunization Advisory Center for updated information.

